A slightly adapted summary of the recommendations from:
[important]The use of echocardiography in acute cardiovascular care: Recommendations of the European Association of Cardiovascular Imaging and the Acute Cardiovascular Care Association 2015.[/important]
The document is a great read for the accomplished echo practitioner, with good use of images and clips.
Indicative echo signs in acute conditions – table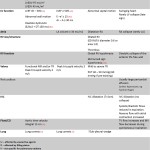
Consider this before interpreting findings:
Definition of ‘normal range’ in the critical care setting
(lack of accurate data, exclusion of many patients from studies/randomized controlled trials)
Your competency
Keep your scan focused if you’re doing a ‘focused assessment’
Qulaity of equipment
Respiratory issues
Mechanical circulatory support
Differential effects on right and left heart
O2 and CO2 levels
Extracorporeal respiratory support
Cardiovascular issues
Filling and inotropic status
Effects of sedation, metabolic status on myocardial function
Acute chest pain
Do echo:
- Echo during pain if suspected myocardial ischaemia (if non-diagnostic ECG and cardiac necrosis biomarkers).
- In underlying cardiac disease (valvular, pericardial or primary myocardial disease);
- If haemodynamic instability unresponsive to simple therapeutic measures;
- In suspected acute aortic syndromes, myocarditis, pericarditis or pulmonary embolism.
Don’t do:
- If non-cardiac aetiology is apparent;
- If confirmed diagnosis of myocardial ischaemia/infarction
Suspected pericardial disease
Do echo:
- In suspected effusion, constriction or effusive-constrictive process;
- If pericardial friction rubs develop in acute myocardial infarction accompanied by symptoms such as persistent pain, hypotension, and nausea;
- For suspected bleeding in the pericardial space (i.e. trauma, perforation);
- For guidance and follow-up of pericardiocentesis.
Acute dyspnoea
Do echo:
- For distinguishing cardiac vs. non-cardiac aetiology of dyspnoea;
- For assessment of LV size and function in suspected HF;
- For determining the cause of failure to wean from mechanical ventilation.
Emergency echocardiographic evaluation in patients with suspected cardiomyopathies
- Calculate 2D LV ejection fraction and additional signs of LV systolic dysfunction (sphericity index, pulsed tissue Doppler derived s’ velocity of mitral annulus, indexed stroke volume).
- Assess LV geometry and regional differences in wall thickness.
- Estimate LV filling pressure (E–e′ ratio, AR – A duration difference, LA volume index, pulmonary arterial systolic pressure).
- Assess reduction of GLS, even if normal ejection fraction.
- Actively diagnose/exclude LVOT obstruction in patients with HCM/LV hypertrophy.
- Take cardiorespiratory support into account.
Suspected/confirmed pulmonary embolism
Do echo:
- In shock or hypotension but CT is not immediately available;
- For cardiac vs. non-cardiac aetiology of dyspnoea when clinical and laboratory clues are ambiguous;
- For therapeutic options in patients with pulmonary embolism at intermediate risk.
Reasonable to do:
- To search for clots in the RA, RV or PAs;
- For risk-stratification.
Don’t:
- For elective diagnostic strategy in haemodynamically stable, normotensive patients with suspected pulmonary embolism.
Shock
Do echo:
- For differential diagnosis
- To choose and guide appropriate therapy, including surgical intervention when indicated.
Cardiac murmur
Do echo:
- If clinical heart failure, myocardial ischaemia/infarction, syncope, thromboembolism, infective endocarditis, or clinical evidence of structural heart disease;
- Where mitral regurgitation is suspected in a patient on positive pressure ventilation, stress echocardiography (volume and/or pressure loading) may be indicated;
- In patients with critical aortic stenosis and cardiogenic shock, to assess suitability for BAV;
- In severe mitral stenosis and cardiogenic shock or pulmonary oedema
- In patients requiring extracorporeal mechanical circulatory support.
Acute traumatic aortic injuries
Do echo:
- In suspected acute traumatic aortic injury; TOE is first-line (with CT).
- Intraoperatively to guide surgical and anaesthesic decisions.
Don’t:
- If cervical spine fractures – relative contraindication.
Suspected acute traumatic cardiac injuries
Do echo:
- Focused assessment immediately in isolated chest trauma, hypotension and tachycardia to exclude pericardial tamponade or tension PTX.
- To diagnose and guide filling in isolated chest trauma, no cardiac tamponade or PTX but having persistent tachycardia or hypotension, signs of HF, abnormal auscultatory findings, abnormal ECG tracings or recurrent arrhythmias.
- TOE is superior to TTE.
Don’t:
- In patients with minor chest injuries and no tachycardia, hypotension, respiratory difficulty, chest pain or other concerning symptoms.
“Echocardiography has become the primary imaging tool for bedside diagnosis and monitoring of patients in acute cardiovascular condi-tions. It is non-invasive, rapid and accurate assessment of cardiac morphology and haemodynamics under stressful situations is very useful in assisting therapeutic procedures. The fact that echocardiography can be repeated when required makes it highly useful in emergency/critical care circumstances”

1 ping
[…] Mandeville from ICMWK has posted a beautiful succinct summary of the European Association of Cardiovascular Imaging’s recent consensus guidelines on the use of […]